When something feels urgent, most people default to the same decision. They go to the closest emergency room and expect to be seen quickly.
That assumption is where the delay begins.
Emergency departments do not operate on distance. They operate on system load. At any given moment, one hospital may be absorbing a surge of high-acuity patients while another is moving steadily with available capacity. From the outside, both look identical. Inside, they function completely differently.
At Innomed, we treat this as a visibility problem, not an access problem. Patients are not lacking options. They are lacking real-time insight into which option will actually move them through care faster. The difference between a short visit and a multi-hour delay is often decided before you leave home.
Quick Answer:
The fastest way to find the nearest ER or walk-in clinic with the shortest wait time is to check real-time wait data before leaving home using tools like WaitlessER, hospital dashboards, or direct calls. The closest ER is often not the fastest. Choosing based on current system load instead of distance can reduce total wait time by hours.
What Actually Determines ER Wait Time
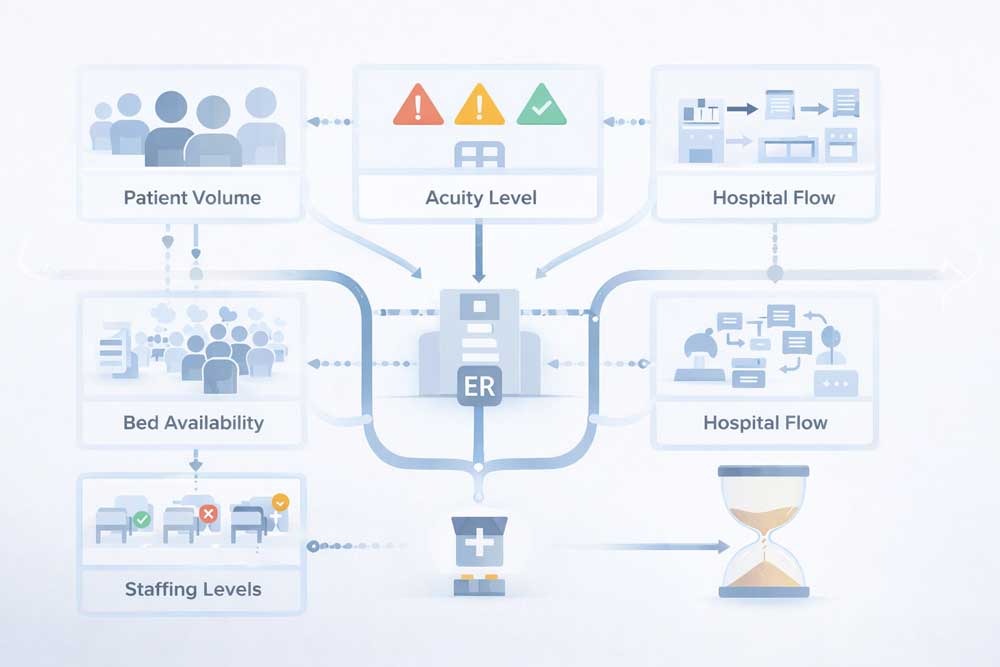
ER wait time follows operational constraints. It is not random, and it is not evenly distributed across facilities.
Each of these factors shifts throughout the day. They interact in ways that compound delays. A hospital with moderate volume but limited beds can move slower than a busier hospital with efficient discharge flow. This is why proximity fails as a decision strategy.
Patients do not experience these variables directly. They experience the outcome as waiting. Without visibility into these constraints, the choice of where to go becomes guesswork.
Why Finding the Right ER Matters
Choosing the right facility changes the entire trajectory of your visit. It affects how quickly you are triaged, when you see a physician, and how long you remain in the system.
Not All ERs Operate at the Same Capacity
Emergency departments run under different conditions at any given time. One may be handling multiple trauma cases. Another may be processing lower-acuity patients with stable flow. The difference is not visible from the outside.
When you enter a high-load ER, you join a queue shaped by severity, not arrival time. This creates long delays for patients with non-critical conditions. In contrast, a lower-load ER processes patients more consistently, reducing total time spent waiting.
The variation is constant. It changes hour by hour. Without checking conditions, patients default to proximity and accept unpredictable outcomes.
Driving Slightly Further Can Change the Outcome
A small increase in travel time often produces a large reduction in total visit time. This happens because wait time is not linear. Once capacity is reached, delays increase rapidly.
A hospital operating near its limits cannot absorb new patients efficiently. Every additional arrival extends the queue. A nearby hospital with available capacity processes patients faster across every stage, from triage to discharge.
Choosing based on load rather than distance shifts the entire experience. It turns a reactive decision into a controlled one.
3 Ways to Check ER Wait Times Before You Leave Home
The goal is simple. Replace assumption with information. The tools are straightforward and accessible.
Method 1: Use the WaitlessER App
WaitlessER provides a real-time view of nearby emergency rooms and walk-in clinics. It aggregates current patient data and historical patterns to produce estimated wait times.
When you open the app, it identifies your location and lists nearby facilities. Each facility is paired with an estimated wait duration. This allows immediate comparison across multiple options.
The value lies in visibility. Instead of committing to a single hospital based on distance, you evaluate the current state of the system and choose accordingly.
Method 2: Call the Hospital Directly
A direct call to the emergency department offers a quick snapshot of current conditions. Staff can indicate whether the department is experiencing delays, operating at normal levels, or under significant pressure.
The response is not precise. It does not provide exact wait times. It provides direction. In many cases, that direction is enough to avoid a high-delay environment.
This method remains effective because it bypasses assumptions. It replaces uncertainty with a direct signal from within the system.
Method 3: Check Hospital Websites
Some hospitals publish live wait time dashboards. These dashboards display estimated wait durations, patient volume indicators, or status updates.
When available, they offer a reliable source of information before leaving home. They reflect internal data and are updated regularly.
The limitation is coverage. Not all hospitals provide this level of transparency. When they do, it becomes a strong input for decision-making.
How WaitlessER Shows You Real-Time Wait Estimates
Understanding how wait time estimates are generated helps you interpret them correctly.
The system combines several data sources. It considers current patient volume, historical flow patterns, and throughput metrics. It then produces an estimated wait duration that reflects likely conditions at that moment.
The process is continuous. As new patients arrive and others are discharged, the estimate updates. This dynamic adjustment provides a near real-time view of system load.
Estimates are not guaranteed. Emergency departments prioritize critical cases. A sudden influx of high-acuity patients can extend wait times quickly. The purpose of the estimate is not precision. It is a comparison. It allows you to choose the best available option at a given moment.
This distinction is important. The tool does not eliminate uncertainty. It reduces it enough to support better decisions.
ER vs Walk-In Clinic: Which One Do You Actually Need
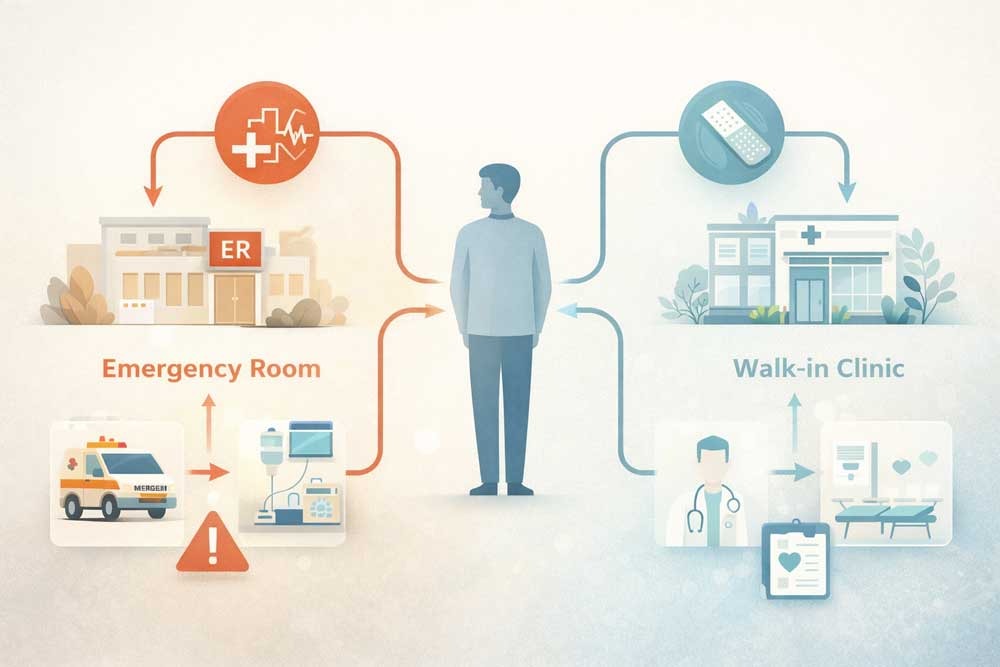
A large portion of ER congestion comes from misaligned demand. Patients often choose emergency care for conditions that could be handled elsewhere. This increases pressure on the system and extends wait times for everyone.
Emergency rooms are designed for life-threatening or severe conditions. Walk-in clinics are designed for lower-acuity cases that require prompt but not critical care.
If symptoms involve chest pain, breathing difficulty, signs of stroke, or severe injury, the ER is the correct choice. These cases require immediate evaluation and access to advanced resources.
If symptoms are stable and non-urgent, a walk-in clinic provides faster and more appropriate care. Clinics operate under different constraints. They process patients in a more predictable flow, without the need to prioritize critical cases over others.
Choosing the correct entry point reduces system friction. It shortens your own wait and supports overall system efficiency.
Which One Should You Choose? (Decision Matrix)
A Simple Decision Framework
Patients benefit from a clear mental model before making a decision.
If the condition feels severe, unpredictable, or life-threatening, go to the ER without delay. In these cases, speed of access to emergency resources outweighs any consideration of wait time.
If the condition is stable and manageable, consider a walk-in clinic first. The total time to care is often shorter, and the environment is better suited to non-critical treatment.
If the situation falls between these two categories, check wait times across nearby ERs and clinics. Choose the option with lower system load.
This framework shifts the decision from habit to intention. It aligns the level of care with the nature of the condition.
Tips for a Faster ER Visit

Once the facility is chosen, several factors influence how quickly you move through the system.
Arrival timing plays a role. Early morning hours often have lower patient volume compared to evenings. Weekends and late nights tend to experience higher demand.
Clear communication during triage also matters. Describing symptoms accurately helps clinical staff assign the correct priority level. This does not change medical urgency, but it reduces delays caused by incomplete information.
Having identification and relevant medical details ready reduces administrative friction. It allows the intake process to move without interruption.
These factors do not eliminate waiting. They reduce avoidable delays within the process.
Why ER Wait Times Spike When You Least Expect It
Most patients assume wait time is based on how many people are ahead of them. That is not how emergency departments work.
ERs operate on a priority system, not a queue. When a critical patient arrives, the system reallocates resources instantly. Staff, rooms, and attention shift toward that case. This does not just delay the next person in line. It reshapes the entire flow of the department.
This is where wait times become unpredictable.
A patient who arrives with a stable condition may be assessed quickly but then wait much longer for treatment. This happens because high-acuity cases continue to enter the system and take precedence. The result is a form of hidden congestion where the waiting room does not look full, but treatment capacity is already committed.
Another factor is inpatient bottlenecks. When admitted patients cannot move to hospital beds, they remain in the ER. This reduces available treatment space for new arrivals. From the outside, nothing changes. Inside, capacity is already consumed.
This is why wait times can double after you arrive. It is not about how many people you see. It is about how the system reallocates resources in real time.
Understanding this changes how you approach the decision. You are not choosing a location. You are choosing the system state you are about to enter.
Why Most Patients Get This Wrong
The common mistake is simple. Patients treat ER selection as a location problem.
This approach ignores the underlying system dynamics. It assumes uniform conditions across facilities, which does not reflect reality.
When patients default to the closest hospital, they enter the system without context. They accept whatever load exists at that location. In many cases, this leads to extended waiting periods that could have been avoided.
The alternative is not complex. It requires a short check before leaving home. That check introduces visibility. Visibility enables choice. Choice changes outcomes.
The System Perspective
From a system perspective, better patient decisions improve overall flow.
When patients distribute themselves based on real-time conditions, pressure is balanced across facilities. Overloaded ERs receive fewer non-critical arrivals. Underutilized facilities absorb more demand.
This redistribution improves efficiency across the network. It reduces extreme wait times and creates more consistent patient flow.
At Innomed, this is where operational insight becomes valuable. Small decisions at the patient level scale into meaningful system-level improvements. Information, when accessible, changes behavior. Changed behavior improves outcomes.
Final Thoughts
Finding the nearest ER is easy. Finding the fastest path to care requires a different approach.
Distance is a visible factor. System load is not. The absence of visibility leads to poor decisions. The presence of even basic information changes those decisions immediately.
Checking wait times before leaving home takes less than a minute. That minute often saves hours. It turns an uncertain process into a controlled one.
In urgent situations, control matters.
Frequently Asked Questions
Is there an app that shows ER wait times?
Yes. WaitlessER provides estimated wait times for emergency rooms and walk-in clinics based on current system conditions.
Are ER wait time estimates accurate?
They are based on real-time data and historical patterns. Actual wait times can change depending on incoming critical cases.
Can I go to any ER or do I need to go to a specific one?
In Canada, you can visit any emergency room regardless of where you live.
Is a walk-in clinic faster than an ER?
For non-emergency conditions, walk-in clinics are usually faster because they handle lower-acuity cases.
What is the most effective way to reduce ER wait time?
Check wait times before leaving home and choose a facility with lower current load instead of the closest one.


.jpg)




