Medical errors are not rare incidents in healthcare systems. They are part of daily hospital operations. They happen in busy emergency rooms, during late-night shifts, and across complex care transitions. At Innomed, we see the same pattern across hospitals in North America. The issue is not lack of expertise. It is how systems handle information under pressure.
AI is changing that structure. It does not replace clinicians. It reduces the gaps where mistakes happen.
Short Answer:
AI reduces medical errors by continuously analyzing patient data, validating clinical decisions, and flagging risks before they reach the patient. It acts as a real-time safety layer across medication, diagnosis, and monitoring. Hospitals that integrate AI through solutions like those developed at Innomed are not removing human judgment. They are reducing the probability of human error.
How Common Are Medical Errors?

Medical Errors by the Numbers (North America Focus)
The scale of these numbers is not theoretical. It reflects consistent findings across multiple healthcare systems and research bodies. Analyses from Johns Hopkins Medicine have highlighted how medical errors rank among leading causes of death in the United States. Broader global patient safety patterns reported by the World Health Organization show that adverse events remain a persistent issue across healthcare systems. Further clinical and policy insights from the National Academy of Medicine, along with peer-reviewed research published in BMJ, reinforce the same conclusion. Medical error is not an isolated issue. It is a systemic problem that requires structural solutions.
The Numbers Behind Preventable Mistakes
Medical errors exist at a scale that most patients do not see directly.
Across North America, studies consistently show that preventable medical harm affects a large number of patients every year. These are not extreme or rare cases. They include everyday failures such as incorrect medication doses, delayed diagnoses, missed abnormal lab results, or breakdowns during patient handoffs.
The underlying issue is not a single mistake. It is an accumulation.
Hospitals operate in environments where clinicians must process large volumes of data in limited time. A single patient record can include medications, lab values, imaging results, prior conditions, and ongoing treatments. Multiply that across dozens of patients per clinician, and the cognitive load becomes significant.
Even experienced professionals cannot manually track every variable at every moment.
This is where AI introduces structural change.
Instead of relying on memory and manual review, AI systems continuously scan data in the background. They do not get fatigued. They do not lose focus. They operate as a parallel layer that watches for inconsistencies, risks, and emerging patterns.
The impact is not dramatic in a single moment. It is cumulative across thousands of decisions.
Types of Errors AI Is Designed to Address
Medical errors are often categorized based on where they occur in the care process.
Medication errors are among the most common. These include incorrect drug selection, dosage issues, or interactions between multiple prescriptions. These errors often happen because patient medication histories are complex and constantly changing.
Diagnostic errors are another major category. These involve missed, delayed, or incorrect diagnoses. In many cases, the issue is not lack of knowledge. It is the difficulty of identifying subtle patterns within large datasets.
Patient identification errors occur less frequently but carry high risk. These involve situations where a procedure, medication, or test is applied to the wrong patient due to identification mismatch.
Monitoring failures also contribute to harm. Patients can deteriorate gradually, and early warning signs may not be obvious without continuous analysis.
Finally, communication breakdowns during handoffs create risk. When patients move between departments or shifts, critical information can be lost or misinterpreted.
AI is not limited to one of these areas. It works across all of them by strengthening how information is processed and shared.
How AI Changes the Structure of Clinical Decision-Making
Traditional hospital workflows depend heavily on sequential review.
A clinician examines a patient, orders tests, reviews results, and makes decisions. Each step depends on the previous one, and each relies on human attention at a specific point in time.
This model works, but it has limitations. If something is missed at one stage, it may not be caught until later, if at all.
AI introduces a parallel model.
Instead of waiting for a specific step, AI systems continuously analyze incoming data. Every new lab result, vital sign, or medication update is evaluated in context with existing data. This creates a system where risk detection is not tied to a single moment.
It becomes continuous.
For example, consider a patient whose condition is slowly deteriorating. In a traditional workflow, this may only become obvious when symptoms become severe enough to trigger intervention. With AI, subtle changes in vital signs and lab trends are analyzed over time. The system identifies patterns that indicate risk before symptoms escalate.
This does not replace clinical judgment. It changes when and how information is surfaced.
Clinicians are not asked to search for signals. Signals are brought to them.
Early Detection as the Core Advantage
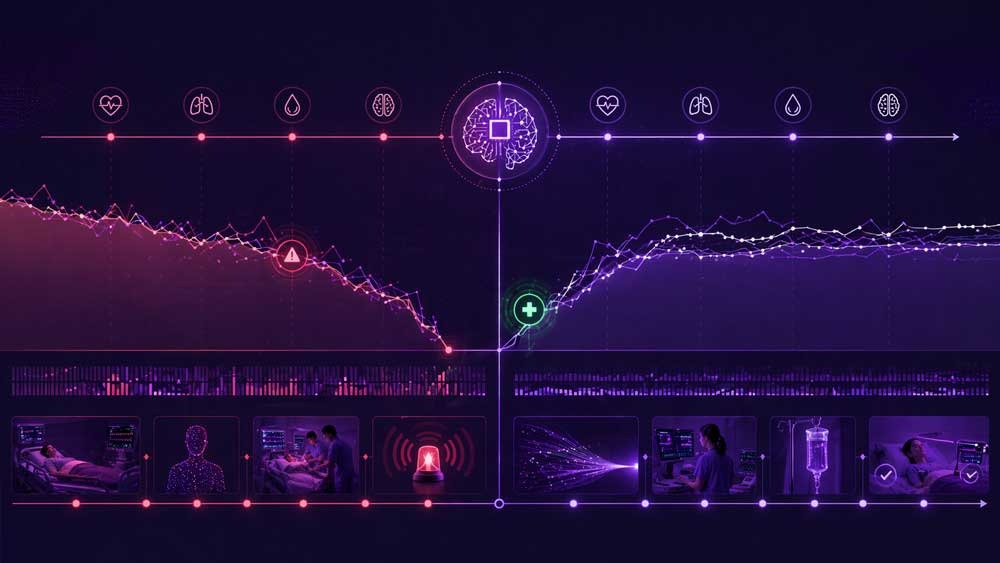
One of the most important contributions of AI in hospitals is timing.
Most medical errors are not caused by completely wrong decisions. They are caused by delayed decisions. A diagnosis that comes hours too late. A medication adjustment that happens after complications begin. A deterioration that is recognized after it becomes critical.
AI shifts detection earlier in the timeline.
This is especially important in conditions like sepsis, where early intervention significantly improves outcomes. The early signs of sepsis are often subtle and distributed across different data points. A slight increase in heart rate, a minor change in lab values, and a shift in temperature may not trigger immediate concern when viewed separately.
AI evaluates these signals together.
By identifying patterns that indicate risk, the system alerts clinicians earlier than traditional methods. This reduces the time between detection and intervention.
The same principle applies to other conditions such as respiratory decline, cardiac events, or complications after surgery.
Early detection does not guarantee perfect outcomes. It increases the window for effective action.
Reducing Cognitive Load in High-Pressure Environments
Hospitals are high-pressure environments by design.
Emergency departments handle unpredictable patient volumes. Intensive care units manage complex cases that require constant monitoring. Even general wards deal with multiple patients with varying levels of risk.
In these settings, cognitive load becomes a limiting factor.
Clinicians must prioritize tasks, manage interruptions, and make decisions quickly. This creates conditions where small details can be overlooked, not because of lack of skill, but because of competing demands.
AI reduces this load by filtering information.
Instead of presenting all data equally, AI systems highlight what requires attention. They identify which patients are at higher risk, which lab results are abnormal in a meaningful way, and which changes require immediate action.
This does not remove the need for clinical expertise. It directs that expertise more effectively.
When clinicians spend less time searching for relevant information, they spend more time making informed decisions.
From Reactive Care to Proactive Systems
Traditional healthcare systems are largely reactive.
A problem appears. It is identified. Then it is treated.
AI introduces a more proactive approach.
By analyzing trends and predicting risk, AI systems allow hospitals to intervene before problems fully develop. This is a fundamental shift in how care is delivered.
For example, instead of waiting for a patient to show clear signs of deterioration, the system identifies early indicators and prompts intervention. Instead of reacting to a medication error after it occurs, the system prevents it during the prescribing phase.
This shift does not eliminate all errors. It changes the probability distribution.
Fewer errors reach the patient. More risks are managed earlier.
At Innomed, this is the focus of AI integration. Not adding complexity, but reducing failure points across the care process.
Where AI Has the Most Immediate Impact
AI adoption in hospitals does not happen uniformly across all departments.
The most immediate impact is seen in areas where data volume is high and timing is critical.
Emergency departments benefit from AI-assisted triage and prioritization. Patients are assessed more quickly, and high-risk cases are identified earlier.
Inpatient care benefits from continuous monitoring systems that track patient status and alert teams to deterioration.
Pharmacy and medication management systems use AI to validate prescriptions and reduce interaction risks.
Radiology integrates AI to assist in image analysis, ensuring that critical findings are not overlooked in high-volume workflows.
These are not isolated improvements. They form a connected system where data flows more effectively between departments.
When these systems are integrated properly, the overall error rate decreases.
5 Ways AI Catches Mistakes Humans Miss
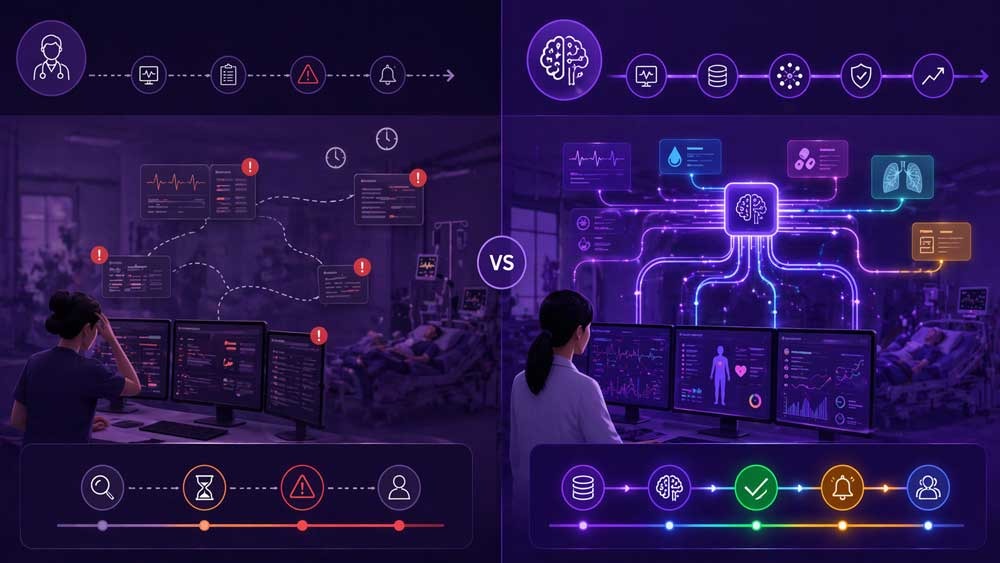
Human vs AI in Error Detection
AI does not replace clinical judgment. It reduces the chances of critical details being missed.
In hospital environments, most errors are not caused by lack of knowledge. They happen because of overload, timing, and fragmented data.
This is where AI has the most direct impact. It acts as a second layer of validation across the care process.
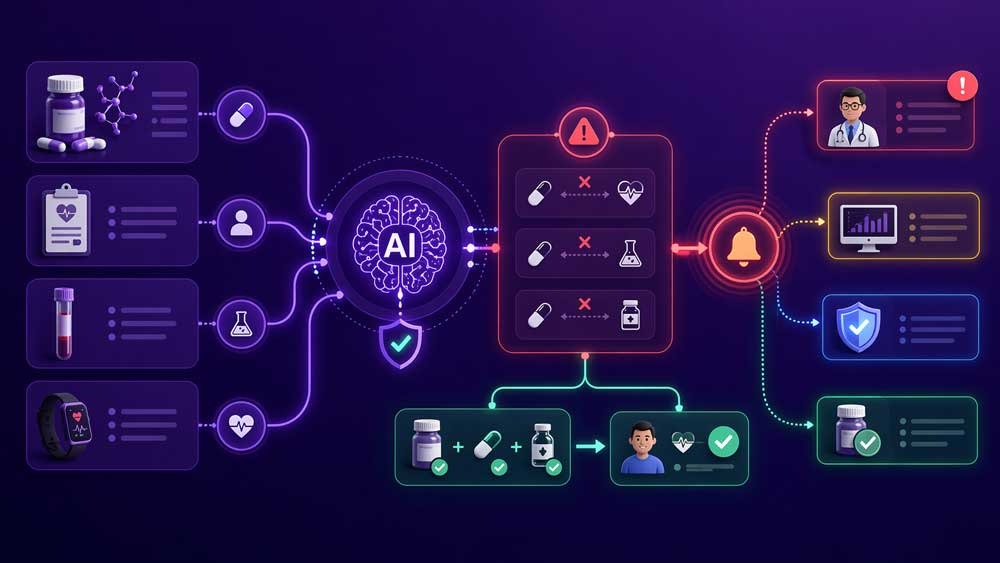
Drug Interaction and Dosage Checks
Medication safety is one of the earliest areas where AI delivered measurable impact.
In a typical hospital setting, a single patient may receive multiple medications across different departments. Each drug carries its own dosage rules, interaction risks, and contraindications based on patient-specific factors such as kidney function, age, or existing conditions.
The traditional system relies on manual review supported by static rules. This works in simple cases. It becomes fragile when patient profiles grow more complex.
AI changes how this validation happens.
Instead of checking prescriptions in isolation, AI systems evaluate the entire medication context in real time. Every new prescription is cross-checked against current medications, lab values, and patient history.
If a risk appears, the system flags it before the medication reaches the patient.
This reduces three common failure points. Incorrect dosage calculations. Overlooked drug interactions. Delayed adjustments when patient conditions change.
The impact is not theoretical. Hospitals that integrate AI-driven medication validation report measurable reductions in adverse drug events.
Lab Result Anomaly Detection
Hospitals generate continuous streams of lab data. The challenge is not access to information. It is recognizing which signals matter at the right time.
A single abnormal value does not always indicate a problem. Trends do.
AI systems focus on pattern recognition across time. They analyze how values evolve rather than how they appear at a single moment.
For example, a slow decline in kidney function may not trigger immediate concern when each individual result falls within acceptable limits. When those results are analyzed together, a clear pattern of deterioration emerges.
AI identifies these patterns earlier than manual review.
It highlights anomalies that are statistically significant in context, not just outside standard ranges.
This changes response timing. Instead of reacting after a condition worsens, clinicians intervene earlier.
Wrong-Patient and Wrong-Site Alerts
Patient identification errors are rare compared to other categories. When they occur, the consequences are severe.
These errors often happen in environments where speed and volume intersect. Emergency care, operating rooms, and imaging departments.
Traditional safeguards rely on manual verification steps. Wristband checks, verbal confirmation, and documentation matching.
These steps are necessary. They are not immune to human error.
AI strengthens this layer by integrating identification checks into the workflow itself.
Before a medication is administered or a procedure is performed, the system verifies that all relevant data points align. Patient identity, medical orders, location, and procedure details.
If inconsistencies appear, the system interrupts the process.
This does not replace existing protocols. It reinforces them at the system level.
Sepsis and Deterioration Early Warnings
Sepsis remains one of the most time-sensitive conditions in hospital care.
Outcomes depend heavily on how early the condition is identified and treated. The difficulty lies in early detection. Initial symptoms are often subtle and distributed across multiple data points.
AI systems monitor patient data continuously. Vital signs, lab values, and historical data are analyzed together.
Instead of waiting for a clear clinical picture to form, the system detects patterns associated with early sepsis.
This allows clinicians to intervene during the early phase, when treatment is more effective.
The same approach applies to other forms of clinical deterioration. Respiratory decline. Cardiac instability. Post-operative complications.
AI shifts the detection window earlier. That shift alone reduces the likelihood of severe outcomes.
Handoff Communication Gaps
Many medical errors do not happen during treatment. They happen during transitions.
Shift changes. Department transfers. Discharge processes.
In these moments, responsibility moves from one team to another. Information must move with it.
When communication is incomplete or inconsistent, risk increases.
AI systems address this by structuring and prioritizing information during handoffs.
Instead of relying on free-form notes or memory, critical data is organized and highlighted. Changes in patient status, pending tests, and active risks are surfaced clearly.
This creates consistency across transitions.
The result is not better communication in a general sense. There are fewer gaps where important details are lost.
Real Examples of AI Preventing Harm

AI in healthcare is no longer experimental. It is already integrated into clinical workflows across North America.
In emergency departments, AI-assisted triage systems analyze patient data before the first clinical interaction is complete. High-risk cases are identified earlier, which improves prioritization.
In radiology, AI tools review imaging scans and highlight suspicious areas. Radiologists still make the final interpretation. The system ensures that critical findings are less likely to be missed in high-volume environments.
In inpatient care, continuous monitoring systems track subtle changes in patient condition. When risk thresholds are reached, alerts are triggered before visible deterioration occurs.
At Innomed, the focus is not on isolated tools. It is on connecting these systems so that data flows without friction. When systems operate in isolation, errors persist. When they operate as a connected structure, risk decreases.
Why AI Does Not Eliminate All Errors
AI improves detection and reduces risk. It does not remove uncertainty from healthcare.
Hospitals are complex systems. Not every scenario is predictable, and not every decision can be automated.
Understanding these limits is critical to using AI safely and effectively.
Limitations of Current AI Systems
AI improves detection and validation. It does not remove uncertainty from healthcare.
Several limitations remain.
AI systems depend on data quality. If input data is incomplete or inaccurate, outputs are affected.
Alert fatigue is another concern. If systems generate too many low-value alerts, clinicians may begin to ignore them. This reduces effectiveness.
Not all clinical scenarios follow predictable patterns. Rare conditions and edge cases still require human interpretation.
AI also depends on integration. In fragmented systems, its ability to analyze complete patient context is limited.
These limitations do not negate the value of AI. They define how it must be implemented.
The Human Factor Remains Central
Clinical decision-making extends beyond data.
Physicians consider patient behavior, context, and factors that are not always captured in structured data. Experience also plays a role. Pattern recognition developed over years cannot be fully replicated.
AI supports this process. It does not replace it.
The most effective model is collaborative. AI reduces noise and highlights risk. Clinicians interpret and decide.
This combination produces safer outcomes than either approach alone.
What You Can Do as a Patient
Patient involvement remains an important part of safety.
Even in systems supported by AI, active participation reduces risk.
Patients who confirm their identity, ask about medications, and understand their treatment plans add an additional layer of verification.
Clear communication with healthcare providers also helps ensure that important information is not missed.
AI strengthens the system. Patient awareness strengthens it further.
Frequently Asked Questions About AI and Errors in Hospitals
How many medical errors happen each year?
Estimates indicate that hundreds of thousands of patients are affected by preventable medical errors annually in North America. The exact number varies depending on methodology, but the scale remains significant.
Can AI completely prevent medical errors?
AI reduces the likelihood of errors by improving detection and validation. It does not eliminate all risk. Human oversight remains essential.
Should patients be concerned about AI making mistakes?
AI systems are designed to support clinical workflows and undergo extensive validation. They do not operate independently. They add a layer of safety rather than replacing existing safeguards.
Does AI replace doctors in hospitals?
AI assists with data analysis and pattern recognition. Clinical decisions remain the responsibility of healthcare professionals.
Where is AI used most in hospitals today?
AI is widely used in medication safety, patient monitoring, radiology, and emergency triage. These areas benefit most from real-time data analysis and early risk detection.






