If you have spent hours in an emergency waiting room, you have already seen a stressed system in action. Across Canada and the United States, emergency departments are absorbing more patients, more complexity, and more operational pressure than many were built to handle.
For patients, the experience feels simple. You arrive, register, wait, and hope your name is called soon. But inside the hospital, emergency wait time is rarely caused by one slow step. It is usually the result of a chain of delays across triage, diagnostics, bed availability, staffing, and discharge coordination.
At Innomed, we treat ER delays as more than a patient frustration issue. They are a signal of how well, or how poorly, a healthcare system is moving people through care.
Direct Answer: Why Are ER Waits So Long?
ER wait times are usually long because patients keep arriving while hospital capacity stays limited. One of the biggest causes is boarding, where admitted patients remain in the ER because no inpatient beds are available. This blocks treatment spaces and slows care for new arrivals.
The problem gets worse when staffing is thin, diagnostics are delayed, and hospitals lack real-time visibility into patient flow. At Innomed, we see this as more than a waiting-room issue. It is a coordination problem across patient flow, capacity, and decision timing., where better routing, visibility, and access tools like Waitless ER help reduce congestion before it escalates.
Quick Overview Table
How Long Do People Actually Wait in the ER?
Emergency wait time is often misunderstood because it refers to several different stages of a visit. Patients are triaged, assessed, tested, treated, observed, discharged, or admitted. Each of those stages has its own timeline.
A patient might be seen by a nurse quickly but then wait much longer for a physician. Another patient might see a clinician relatively fast but spend hours waiting for imaging, laboratory results, or a bed. This is why many people leave the ER saying they “waited all day,” even if the first assessment happened earlier.
From an operational perspective, the most important measure is not only door-to-doctor time. It is the total length of stay.
Average Wait Times in Canada and the US
Emergency room wait times vary by region, hospital type, and patient acuity. Still, a broad pattern exists across North America: patients with less urgent conditions wait longer, and total ER stays often extend much further than expected.
In Canada, non-urgent patients commonly wait 2 to 6 hours before physician assessment in busy hospitals, and total visit time may stretch beyond 8 hours when diagnostics or admission are involved. In major urban centres, these delays become more visible during respiratory season, weekends, and holiday periods.
In the United States, physician contact is often faster in many regions, but this does not always translate into a shorter full visit. Patients who need specialist review, imaging, or admission often remain in the department for several hours. In high-volume hospitals, throughput delays still create long stays even when initial triage is efficient.
The key difference is not always how quickly a patient is first seen. It is how efficiently the hospital moves them after that point.
What Most Patients Misunderstand About ER Wait Time
Many patients assume the wait ends when they see a doctor. In practice, that is only one checkpoint.
A typical emergency visit includes several handoffs. After triage, there may be a wait for room placement. After physician assessment, there may be another delay for testing. Once results are available, there may still be a wait for treatment decisions, discharge planning, or inpatient admission.
This means the visible waiting room is only one part of the problem. Much of the delay happens after a patient has already entered the system.
Why Some ERs Are Worse Than Others
Not all emergency departments operate under the same constraints.
Large urban hospitals often receive more complex cases, higher ambulance volumes, and a greater share of vulnerable or high-needs patients. Teaching hospitals may also manage additional layers of clinical coordination. Community hospitals may face the opposite problem, limited inpatient capacity and fewer specialist resources.
Two ERs with similar patient numbers can perform very differently depending on how well they manage staffing, diagnostics, admissions, and discharge flow.
The 5 Biggest Reasons ERs Are Overcrowded
Emergency department overcrowding is rarely caused by a single issue. It results from multiple constraints interacting across the hospital. From an operational perspective, delays happen when patient inflow exceeds the system’s ability to move patients through assessment, treatment, and disposition. Even small inefficiencies at each stage can accumulate and create visible congestion.
Not Enough Beds and Staff
One of the clearest causes is simple capacity mismatch. When too many patients arrive and staffing is limited, every stage slows down, from triage to discharge. Bed availability is just as critical. Even a ready clinical team cannot move patients forward without available treatment or inpatient space. This is why ERs can appear full despite continuous activity.
Non-Emergency Patients in the ER
A significant portion of ER visits are not life-threatening. Many patients present with conditions that could be handled in urgent care or primary care settings, especially outside regular hours. When the ER becomes the default entry point, lower-acuity cases compete with true emergencies, increasing overall congestion. This reflects both access gaps and system design challenges.
Patients Waiting for Hospital Admission (Boarding)
Boarding is one of the most impactful drivers of delay. Patients who have been admitted remain in the ER due to lack of inpatient beds, occupying critical treatment space. This creates a cascading effect, slowing new admissions, crowding waiting rooms, and increasing pressure on staff who must manage both emergency and inpatient-level care.
Why Boarding Creates System-Wide Congestion
Boarding is often described as an ER issue, but it is more accurately a hospital-wide throughput failure.
When inpatient units are full, emergency departments become overflow zones. That changes the purpose of the ER. Instead of rapid assessment and transition, it becomes a temporary holding environment.
This also increases cognitive load on clinicians. Emergency staff must care for patients who require inpatient-level monitoring while still managing new acute arrivals. The result is slower turnover, more fragmented attention, and greater operational strain.
Until hospitals improve inpatient flow, emergency departments will continue to absorb this bottleneck.
Seasonal Surges: Flu Season, Holidays, Pandemics
Demand in emergency departments is not constant. Flu season, respiratory outbreaks, and holiday periods increase patient volume while system flexibility decreases. Hospitals already operating near capacity have limited ability to absorb these surges, making delays more visible and harder to manage.
Outdated Systems and Paper-Based Processes
Many ER delays are not caused by major clinical issues. They are administrative.
A patient may be ready for discharge, but transport is delayed. A bed may be available, but its status is not updated. A physician may place an order, but its operational impact is not visible to the next team.
When hospitals rely on disconnected workflows and limited real-time visibility, small inefficiencies accumulate throughout the day. Over time, those minutes become hours.
This is one of the least visible causes of overcrowding, but also one of the most fixable.
What Hospitals Are Doing to Fix ER Wait Times

Hospitals across North America are trying to reduce emergency congestion through operational redesign, staffing changes, and digital support tools. The most effective strategies do not focus only on triage speed. They focus on whole-system throughput.
AI-Powered Patient Flow Systems
Hospitals are increasingly turning to AI and operational intelligence tools to improve emergency throughput. The most effective systems do not simply estimate demand. They help organizations see pressure earlier, route patients more intelligently, and reduce unnecessary congestion before it reaches the waiting room.
This is where real-time flow systems become valuable. Instead of treating ER delay as a front-desk problem, these platforms help hospitals and healthcare networks manage the full pathway around emergency access.
At a practical level, this includes:
- identifying pressure before visible crowding occurs
- surfacing live availability across emergency and urgent care settings
- supporting care guidance before arrival
- improving system responsiveness during peak periods such as flu season or holidays
This operational model aligns closely with how Waitless ER is positioned, as a public-facing emergency access layer built around real-time visibility, patient guidance, and demand-aware optimization
Where AI Actually Makes a Measurable Difference
Not every AI solution improves emergency operations. The useful ones focus on specific friction points.
High-value applications include identifying patients who are medically ready for discharge but delayed by coordination issues, predicting likely admission pressure based on live demand, and helping operations teams prioritize blocked beds or workflow slowdowns.
These tools do not replace clinicians. They improve how quickly the system sees and responds to pressure.
Hospitals that reduce ER delays most effectively usually combine technology with clear escalation processes and accountable operational teams.
Real-Time Wait Time Transparency for Patients
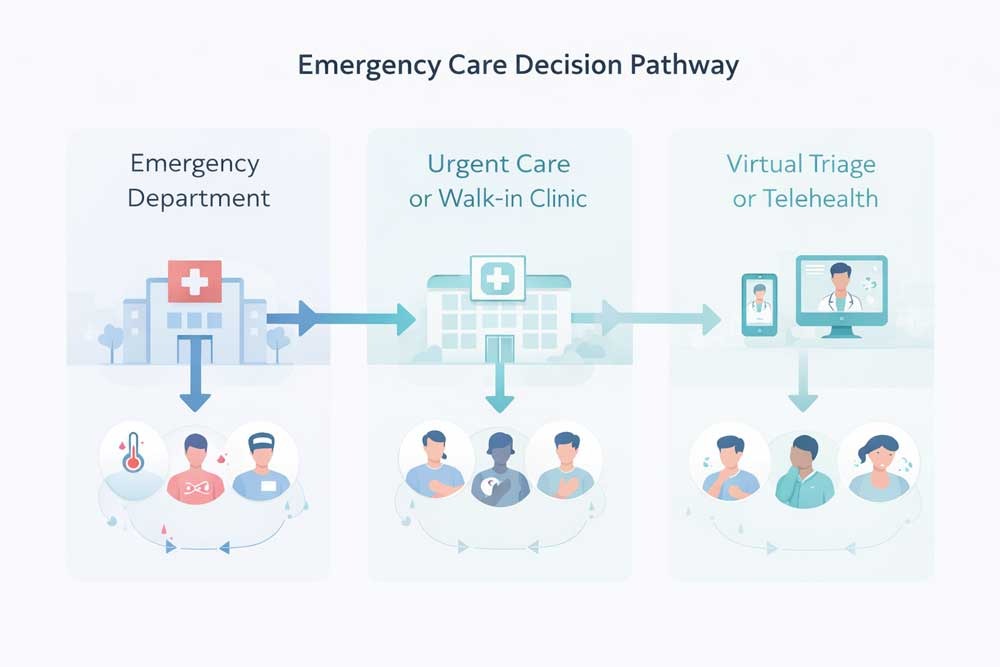
One of the most practical ways to reduce unnecessary ER congestion is to improve visibility before patients arrive.
When people do not know which emergency departments are overloaded, or whether a nearby urgent care option is more appropriate, they tend to choose based on urgency, guesswork, or habit. This increases avoidable pressure on already crowded sites.
Real-time wait time visibility changes that dynamic. It gives patients clearer expectations, reduces uncertainty during stressful moments, and supports better distribution of demand across the care network.
This is one of the clearest strengths of the Waitless ER model. By making emergency and urgent care availability easier to understand, it helps patients make faster and more informed care decisions before congestion worsens.
Virtual Triage Before You Arrive
Many emergency delays begin before the patient even enters the building.
When people are unsure whether they need the ER, urgent care, or another care pathway, they often default to the emergency department. This is understandable, but operationally inefficient.
Virtual triage tools help reduce this friction by guiding patients before arrival. They provide symptom-based direction, support lower-friction decision-making, and reduce unnecessary ER visits by helping people choose a more appropriate entry point when emergency care is not required.
This is also where platforms like Waitless ER become especially useful. Their value is not limited to showing a queue. They support care guidance under pressure, which is often what patients need most in the moment.
What You Can Do to Avoid Long ER Waits
Patients do not control hospital capacity or staffing levels, but they can make more informed decisions about when and where to seek care.
One of the most effective steps is choosing the right entry point based on symptom severity.
In Canada, access options vary by province, but most regions offer some combination of walk-in clinics, urgent care centres, virtual care platforms, and nurse triage services. When these options are available, using them can help reduce unnecessary pressure on emergency departments and shorten wait times for everyone.
Before going to the ER, it is often useful to check provincial wait time dashboards, local hospital updates, or nurse advice lines. These services provide guidance on where to go and what level of care is appropriate based on your situation.
In many cases, tools like Waitless ER make this process easier by offering real-time visibility into emergency and urgent care access. This helps patients make faster, more informed decisions, especially during peak periods such as evenings, weekends, or flu season.
Choosing the right entry point does more than reduce your own wait time. It helps protect emergency capacity for patients who need immediate care and improves how the system functions overall.
Why Choosing the Right Entry Point Matters
Emergency departments are designed for time-sensitive, high-risk conditions.
When lower-acuity cases enter the ER, they do not simply “wait separately.” They still consume registration, triage, space, and clinical review. That creates system friction.
This is why public education, virtual triage, and care navigation matter. Better routing improves both patient experience and system efficiency.
How to Check ER Wait Times Before You Go
Before leaving home, patients should check whether their local region offers wait time dashboards, hospital websites with emergency updates, urgent care finders, or nurse triage lines.
In many cases, mobile tools like Waitless ER make this process easier by providing real-time visibility into emergency and urgent care access, helping patients make faster and more informed decisions under pressure.
Why Fixing ER Wait Times Requires More Than Faster Triage
A common misconception is that emergency delays are mainly a triage problem. They are not.
A hospital can triage patients quickly and still produce long stays if diagnostics are slow, admissions are blocked, and discharge coordination is weak. This is why isolated front-end fixes often fail. They improve the first ten minutes of the visit while leaving the next six hours untouched.
Sustainable improvement requires better coordination across the entire hospital.
That includes bed management, inpatient discharge timing, diagnostic access, staffing visibility, and operational command processes. Without those elements, emergency departments remain vulnerable to the same congestion cycle.
How Smarter Emergency Department Operations Improve Patient Experience

{Find the Fastest ER Now!}
Wait times are usually discussed in terms of efficiency, but they also shape trust.
Patients who wait without updates often feel abandoned, even when care teams are working intensely behind the scenes. Uncertainty increases anxiety. Poor visibility reduces confidence. Delays without explanation make the system feel disorganized.
Better emergency operations improve more than throughput. They improve communication, predictability, and patient perception of care.
The Hidden Cost of Long ER Wait Times
Extended emergency delays affect more than satisfaction scores.
They increase clinical risk by delaying treatment decisions. They contribute to staff fatigue by forcing teams to operate in persistent overload. They reduce resilience because a crowded emergency department has less capacity to absorb the next surge.
Hospitals that improve throughput often see broader benefits across patient safety, clinician workload, and operational stability.
At Innomed, we focus on helping healthcare systems improve patient flow through better visibility and coordination.
Final Thought
Long ER wait times are not a failure of one department. They reflect how the entire system moves, or fails to move, patients through care.
Hospitals that reduce delays do not simply move faster at the front door. They improve visibility, coordination, and decision-making across the full patient journey.
This is where healthcare AI becomes meaningful, not as a standalone tool, but as part of how the system operates.
At Innomed, services and solutions like Waitless ER reflect this shift, helping healthcare systems reduce uncertainty, improve access visibility, and support better emergency flow before pressure escalates.
Frequently Asked Questions About Long Waiting ER Times
What is the average ER wait time in Canada?
For lower-acuity conditions, many patients in Canada wait between 2 to 6 hours before physician assessment, with total visit times often extending much longer in busy hospitals.
Can I check ER wait times before going?
In many regions, yes. Hospital websites, regional dashboards, and digital triage tools increasingly provide wait estimates or care navigation support.
Why do some patients wait longer than others?
Emergency departments use triage, not first-come-first-served order. Patients with more urgent symptoms are treated first regardless of arrival time.
Should I go to the ER or a walk-in clinic?
Walk-in clinics are more appropriate for lower-acuity concerns such as mild fever, sore throat, or minor injuries. Emergency departments are the right setting for severe, time-sensitive conditions.
Does AI really help reduce ER wait times?
It can, when used to improve patient flow, bed coordination, discharge timing, and operational visibility. AI is most effective when it supports clear workflow decisions.







